In the United States, drugmakers have flooded the market with powerful, sophisticated opioids. And that's fueled an epidemic of addiction. But across Africa many patients can't afford even mild painkillers — let alone medications to help people in extreme pain.
Uganda has come up with a solution that goes back to basics with one of the world's original painkillers: morphine.
The government mixes a powdered form of the drug with water to create a drinkable analgesic that officials say has provided patients with effective relief without giving rise to widespread addiction. Just as important, it's cheap.
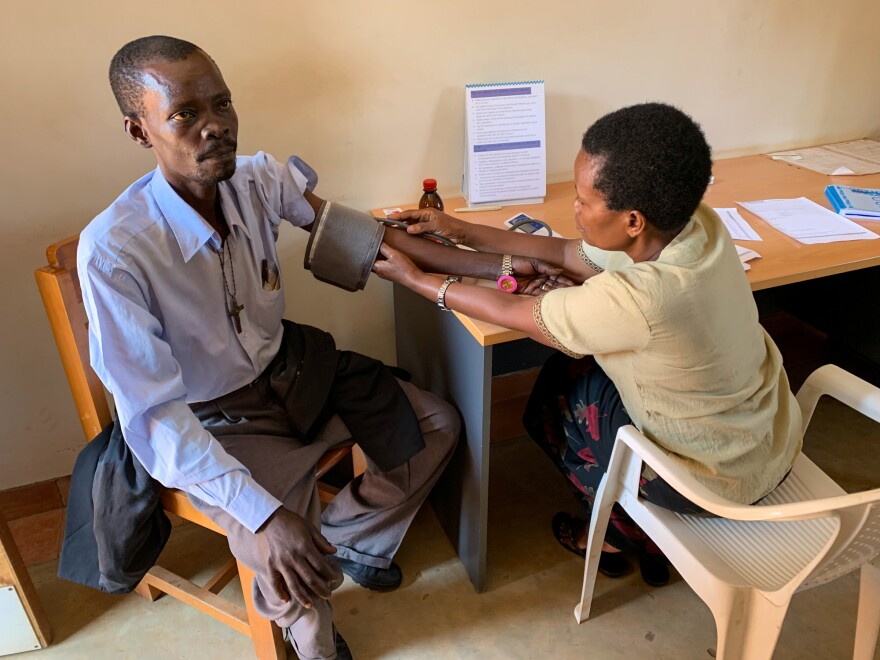
At a medical clinic in the capital, Kampala, Nurse Resty Nakanwagi pulls out two bottles of the stuff and sets them on a table in front of a patient.
"So, this is the morphine," Nakanwagi says. "You are going to take this every four hours, okay? Then at night you make it a double dose."
Nakanwagi typically provides a two-week supply of the liquid for patients to drink at home.
The patient, Justine Nakayenga, nods. She used to work on data entry for an insurance company. Then she got breast cancer that has metastasized. She's 30 years old. But she's lost so much weight, she looks like she could be 12.
Two weeks ago, a tumor reached Nakayenga's spinal cord, causing leg cramps so excruciating that the pain was all she could think about.
"You're like, 'God, please get me through this. Please get me through this,' " she says with a sigh.
Then, two days ago, Nakayenga got her first dose of liquid morphine from this center — a nonprofit called Hospice Africa.
Within hours of drinking the mixture, says Nakayenga, her pain was gone.
"I went and laid down, and — oh my God, the sleep came!" she recalls. "I just drifted away until morning. I'm like, 'Wow, I actually slept until morning!'"
'Look, this is affordable'
In the United States, morphine and other painkillers related to it are routinely given to patients with extreme pain. But those are powerful formulations and delivery systems with price tags to match: Time-release capsules, pumps that give you the right dose with a push of button.
By contrast, the liquid morphine recipe that Uganda uses is low-tech. And that's precisely what makes it useful, says Anne Merriman, founder of Hospice Africa.
"You know, they say it's easier to make than a cup of coffee," she says with a chuckle.

A British nun-turned-doctor, Merriman helped develop Uganda's system for using liquid morphine back in the late 1990s.
"I said, 'Look, this is affordable,' " she says. "It was, at the time, one dollar for 10 days treatment of the average patient."
Today the price is only slightly higher — about $2.50 for a week's supply.
And there's another draw. Merriman says this drinkable morphine has not fostered addiction in Uganda.
"It's so diluted," she says. "It's not going to give you a high. They have to take an awful lot to get any form of a high."
When Merriman first proposed bringing liquid morphine into Uganda, Dr. Ignatius Kakande was one of several local health officials who embraced the idea as a broader solution to the country's shortage of painkillers.

At the time, Kakande was head of surgical training at Uganda's premier medical college. He says he had grown frustrated seeing so many of his patients suffer. Generally the only opioid he could offer was pethidine, a synthetic more commonly known in the United States by its brand name Demerol.
But most patients were unable to afford the opioid on their own. And the government's budget for buying it was equally limited. So it wasn't always in stock. And even when it was, Kakande says, Ugandan law prohibited him from prescribing it outside of a hospital. Once he'd run out of possible cures for his patients, says Kakande, "we were just sending them home to die in pain."
Within months of meeting Merriman, Kakande arranged for Uganda's surgeons to be trained on how to prescribe liquid morphine. As evidence mounted that it was making a difference without producing addiction, Ugandan officials decided to massively increase access.
Among their most high-impact moves was passing a law in 2004 that permits nurses to prescribe the mixture, says Dr. Emmanuel Luyirika. He heads the African Palliative Care Association, a nonprofit based in Uganda that's trying to get more countries to adopt the country's model.
Empowering the nurses was key, says Luyirika, because in Uganda's more rural areas, "the ratio of doctor-to-patient is so poor, you may wait for a year before you ever get a doctor."
Ugandan officials took another important step in 2005, when they decided to provide liquid morphine to patients for free.
In a country where about half of the population was living on less than $2 a day, this made an immediate difference. In the space of a year, the percentage of Ugandans getting the pain medication they need shot up from practically none to 11 percent.
'We don't need a lot of money!'
Unfortunately, in the years since, there's been no further increase in the share of Ugandans gaining access to sufficient pain medication.
"Funding is a major issue," says Luyirika. Overall, he says, Uganda spends very little of its national budget on health care. That includes money for training and deploying nurses to prescribe liquid morphine.
"We need to see the Ugandan government invest more money in health — especially in personnel," says Luyirika.
A related issue, he adds, is that compared to health programs that save lives, efforts to reduce patients' pain are a much lower priority — both for the government and for international donors.
This is maddening to Luyrikia because, he says, pain management through liquid morphine produces so much benefit for so little expense. "We don't need a lot of money!" he says.
A lack of funding is also the main reason few other African nations have followed Uganda's lead, says Luyirika — even as a stream of officials and health experts from more than a dozen African countries have flocked to Uganda to learn about its system for liquid morphine.
"They come here. They see what Uganda does," and sure, a few have even taken inspiration, says Luyirika. Botswana, Rwanda and Swaziland are now covering the cost of liquid morphine for patients, for example. But overall, when it comes to actually getting morphine to patients, the progress has been glacial.
"We have countries in Africa where the amount of morphine that they import meets almost zero [percent] of the need," says Luyirika. And that's not even considering other forms of opioids and analgesics that would be helpful to have available for cases in which morphine is not the most suited.
'It has to be a mindset change'
Dr. Chimwemwe Kabaghe thinks there's another obstacle to the widespread dissemination of liquid morphine that's just as problematic as the shortage of resources: Health workers themselves.
Kabaghe speaks from experience. A doctor from Malawi, she recalls her reaction the first time a colleague suggested she prescribe liquid morphine to a dying patient.
The patient's body was riddled with painful tumors, recalls Kabaghe. "She wasn't eating. She wasn't sleeping. She was just constantly crying in pain."
And with no obvious options available to help her, the woman's screams weren't even getting her much sympathy — and were just stressing the staff out.
"Everyone in the ward was angry with her," says Kabaghe.
Yet when, by chance, the colleague informed Kabaghe that liquid morphine is now legal in Malawi, Kabaghe's overriding instinct was skepticism.
"I'm like, 'Is that safe? Is that okay?' says Kabaghe. "This is a very dangerous drug because it comes from opium. So maybe there's something that's addictive about it. Or maybe it would kill the patient."
It was only because of the colleague's reassurance that Kabaghe bothered doing the research that convinced her liquid morphine was worth a try.
When she saw the peace that the drug brought to her patient, it made Kabaghe rethink her whole approach to medicine.
"I saw how it was really, really beneficial for people to not be in pain," she says.
And she concluded that the shortage of painkillers in Africa has made health workers like her lose sight of the value of simply making sure their patients are comfortable.
Now Kabaghe is on a mission to get Malawi to put more emphasis on palliative care – the branch of medicine that focuses on easing pain, particularly for terminally ill patients.
'I've come to see how it's done'
That's brought Kabaghe to Uganda. The country, she explains on a recent morning, "is like the hub of palliative care. So I've come to see how it's done here."
She's in an SUV, bumping along a rutted road in Kampala, alongside a Ugandan nurse with Hospice Africa whom Kabaghe is shadowing for the day.
The nurse, Josephine Nabitaka, is delivering liquid morphine to patients who are too sick to come into the clinic.
"This is the home," Nabitaka announces as the vehicle slows to stop.
Their first patient is an 81-year-old woman with advanced colorectal cancer. They find her curled up in bed — a mosquito net hanging over her.
Nabitaka speaks to the woman softly, asking if the morphine is still working. Then Nabitaka takes a look at the card where doses are being logged.
"Okay," she says, turning to Kabaghe, the doctor from Malawi. "Whenever we come to the home, before we leave we have to check on their balance of medication."
Kabaghe looks over the log. "It's 2 milliliters? Or is that 2.5?" she asks.
Back in the car, Kabaghe says she's taken a position with Malawi's government as its main contact on palliative care.
"So I'm trying to be the one who will make the Ministry of Health take initiative," she says.
But she expects her main challenge to be getting more of her fellow health workers to recognize the importance of focusing on their patients' pain. Otherwise, she says, the natural response when someone is told about liquid morphine will be the same as hers:
"You're just like, 'Hmm. Nah. Maybe not. Maybe let's just stick to the things that we know.'"
"It has to be a mindset change," she says.
Until that takes place, those championing liquid morphine say they often find themselves ruminating about patients forced to go without.
Chris Ntege is head chemist at the government-funded facility where Uganda's morphine solution is mixed. He's scooping morphine powder from a bag onto a scale with an intent expression.

"Every time I weigh out the powder," he says, "I'm imagining that patient in the village who could be in pain. And you have here a powder that could take away all that pain."
The bag is almost empty. But Ntege keeps scraping.
"I don't want to leave even a small gram inside there," he says.
Copyright 2024 NPR. To see more, visit https://www.npr.org.



